Analysis of risk factors for postoperative liver metastasis in colorectal cancer andconstruction of a predictive model
-
摘要:
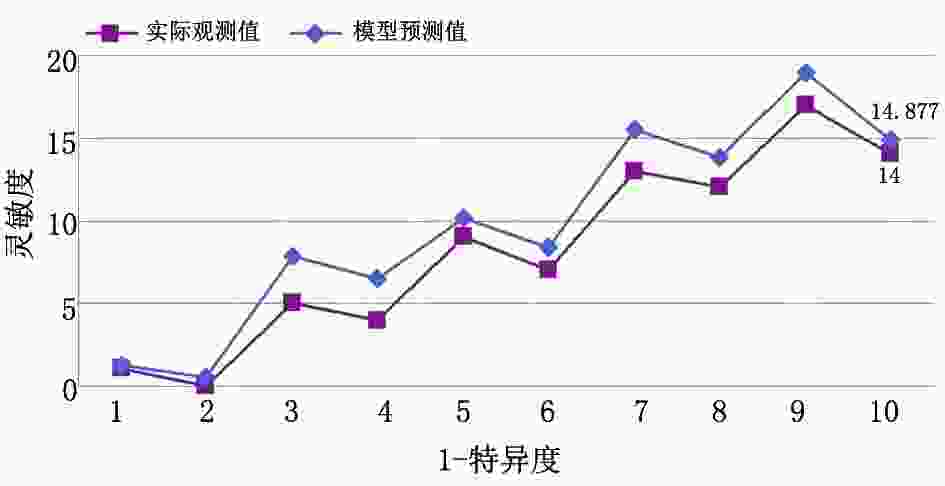
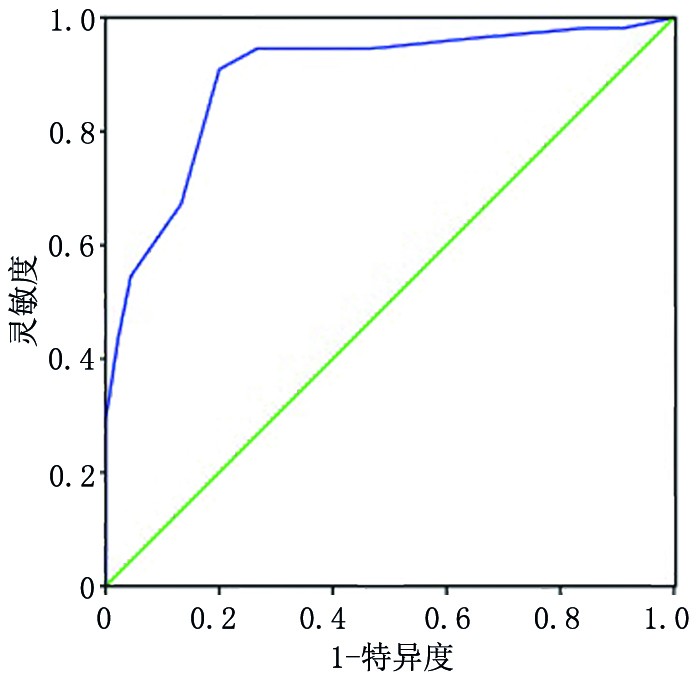
目的 分析结直肠癌术后肝转移的危险因素并构建预测模型。 方法 选取2011年1月至2015年12月于苏州市第九人民医院行根治性手术切除的247例结直肠癌患者作为观察对象,依据随访是否出现肝转移分为转移组、非转移组。对两组各项指标进行单因素筛选,再行Logistic多因素回归分析,并建立预测模型,应用受试者工作特征(receiver operating characteristic,ROC)曲线检测其区分度,应用拟合优度检验评价其校准度。另选本院102例结直肠癌患者进行该模型的临床验证。 结果 247例结直肠癌患者术后随访中出现肝转移81例(转移组),占32.79%,其中分化程度、淋巴结转移、血清癌胚抗原(carcinoembryonic antigen,CEA)、D-二聚体、血清白蛋白(serum albumin,Alb)、可溶性细胞间黏附分子-1(soluble intercellular adhesion molecule-1,sICAM-1)、miRNA-203表达量均是结直肠癌术后肝转移的危险因素(P<0.05)。根据危险因素得出预测模型表达方程为:Logit(P)=1.203×分化程度+2.065×淋巴结转移+1.257×CEA+0.829×D-二聚体+0.395×Alb+1.156×sICAM-1+1.484×miRNA-203表达量-34.187。该模型ROC曲线下的面积为0.895(95% CI:0.830~0.959),最大约登指数(0.722)对应的灵敏度为0.896,特异度为0.904。经拟合优度检验,χ2=3.014,P=0.421。临床验证模型预测的灵敏度为86.21%,特异度为89.04%,准确率为88.24%。 结论 结直肠癌术后肝转移的危险因素分别为分化程度低、淋巴结转移、CEA高表达、D-二聚体高表达、Alb降低、sICAM-1升高、低表达miRNA-203。以此构建预测模型,区分能力良好,可以有效评估结直肠癌术后肝转移风险。 Abstract:Objective To analyze the risk factors for liver metastasis after colorectal cancer surgery and construct a predictive model. Methods In total, 247 colorectal cancer who underwent radical surgical resection at Suzhou Ninth People's Hospital from January 2011 to December 2015 were selected for postoperative observation. These patients were assigned into groups in which metastases did or did not appear. One-way ANOVA of prognostic indicators among both groups was performed. Logistic multiple factor regression analysis was employed, and a predictive model was constructed. Receiver operating characteristic (ROC) curves were analyzed to assess the discrimination of the model, and a goodness of fit test was used to evaluate its calibration. Another 102 colorectal cancer patients in this hospital were selected for clinical validation of the model. Results During follow-up of 247 colorectal cancer patients, 81 cases of liver metastasis (metastasis group) occurred (32.79%). Among these, the degree of differentiation, lymph node metastasis, and expression of serum carcinoembryonic antigen (CEA), D-dimer, albumin (Alb), soluble intercellular adhesion molecule-1 (sICAM-1), and miRNA-203 are all risk factors in colorectal cancer patients for postoperative liver metastasis (P<0.05). According to these risk factors, the equation expressing our predictive model is: Logit (P)=1.203×differentiation degree + 2.065 × lymph node metastasis + 1.257 × CEA + 0.829 × D-dimer + 0.395 × Alb + 1.156 × sICAM-1 + 1.484× miRNA-203 expression level-34.187. The area under the ROC curve for the model was 0.895 (95% CI: 0.830~0.959). The maximum Youden index (0.722) corresponded to a sensitivity of 0.896 and a specificity of 0.904. Goodness of fit test yielded χ2=3.014 and P=0.421. The prediction sensitivity of the clinical validation model was 86.21%. The specificity and accuracy were 89.04% and 88.24%, respectively. Conclusions The risk factors for postoperative liver metastasis in colorectal cancer include reduced differentiation, lymph node metastasis, high CEA expression, high D-dimer expression, decreased Alb level, increased sICAM-1 level, and low degree of miRNA-203 expression. These findings aided in the construction of a predictive model with good discrimination ability that can effectively assess the risk of liver metastasis after colorectal cancer surgery. -
Key words:
- colorectal cancer /
- liver metastasis /
- risk factors /
- prediction model
-
表 1 转移组与非转移组患者的临床资料比较 n(%)
临床特征 转移组(n=81) 非转移组(n=166) χ2/t P 年龄(岁) 1.167* 0.280 <60 32(39.51) 54(32.53) ≥60 49(60.49) 112(67.47) 性别 0.902* 0.342 男 51(62.96) 94(56.63) 女 30(37.04) 72(43.37) 肿瘤最大直径(cm) 2.026* 0.155 ≥5 54(66.67) 95(57.23) <5 27(33.33) 71(42.77) 临床分期(期) 2.988* 0.084 Ⅰ 32(39.51) 85(51.20) Ⅱ 49(60.49) 81(48.80) 分化程度 26.368* <0.001 低 43(53.09) 39(23.49) 中 26(32.10) 58(34.94) 高 12(14.81) 69(41.57) 淋巴结转移 58.301* <0.001 有 75(92.59) 69(41.57) 无 6(7.41) 97(58.43) CEA(ng/mL) 7.05±2.39 6.34±1.92 2.866** 0.004 CA19-9(kU/L) 41.26±15.87 38.75±13.18 1.312** 0.190 D-二聚体(μg/L) 190.34±45.38 178.39±31.74 2.399** 0.017 Alb(g/L) 28.96±5.92 30.67±6.45 2.008** 0.045 sICAM-1(μg/L) 202.45±32.35 192.58±27.93 2.473** 0.014 miRNA-203表达量 1.83±0.51 2.64±0.73 8.971** <0.001 *:采用χ2检验;**:采用t检验;CA19-9:糖类多肽抗原 表 2 结直肠癌术后肝转移的多因素Logistic回归分析
因素 β χ2 P OR(95%CI) 分化程度 1.203 4.648 0.022 3.330(2.054~7.992) 淋巴结转移 2.065 4.857 0.020 7.885(2.094~12.556) CEA 1.257 3.189 0.032 3.515(2.154~7.675) D-二聚体 0.829 3.990 0.033 2.291(1.295~4.856) Alb 0.395 4.277 0.025 1.484(1.026~3.255) sICAM-A 1.156 3.556 0.031 3.177(1.135~4.156) miRNA-203表达量 1.484 5.879 0.015 4.411(2.103~8.297) 常数项 −34.187 13.984 0.001 − 表 3 模型的灵敏度、特异度及准确率 例
模型预
测结果实际结果 合计 灵敏度
(%)特异度
(%)准确率
(%)肝转移 非肝转移 肝转移 25 8 33 非肝转移 4 65 69 合计 29 73 102 86.21 89.04 88.24 -
[1] 赵权权,史晓辉,傅传刚,等.直肠癌新辅助放化疗后淋巴结转移危险因素评估及其临床意义[J].中华胃肠外科杂志,2016,19(9):1040-1043. doi: 10.3760/cma.j.issn.1671-0274.2016.09.017 [2] Gunawardene A, Desmond B, Shekouh A, et al. Disease recurrence following surgery for colorectal cancer: fiveyear follow-up[J]. N Z Med J, 2018, 131(1469):51-58. [3] 常文举,任黎,许剑民.2019 年结直肠癌肝转移诊疗指南最新解读[J].中国普外基础与临床研究,2019,8(26):1-5. [4] 冯磊,徐明清.miR-203与肿瘤关系的研究进展[J].中国普外基础与临床杂志,2017,24(2):259-263. doi: 10.7507/1007-9424.201606045 [5] 邵仟仟,林国乐.2017. V1版《NCCN结直肠癌诊治指南》更新解读[J].中国全科医学,2017,20(6):635-638. doi: 10.3969/j.issn.1007-9572.2017.06.001 [6] 许剑民,任黎.结直肠癌肝转移诊断和综合治疗指南(2016版)[J].中华消化外科杂志,2016,15(8):755-767. doi: 10.3760/cma.j.issn.1673-9752.2016.08.001 [7] 曹毛毛,陈万青.中国恶性肿瘤流行情况及防控现状[J].中国肿瘤临床,2019,46(3):145-149. doi: 10.3969/j.issn.1000-8179.2019.03.283 [8] 李佩,鲁祖斌,严庆波,等.miR-122与结直肠癌术后肝转移的关系[J].中华肝脏外科手术学电子杂志,2020,9(4):385-388. doi: 10.3877/cma.j.issn.2095-3232.2020.04.020 [9] 何伟,吴琼.结直肠癌肝转移的危险因素分析[J].内蒙古医科大学学报,2019,41(4):340-343. [10] Campos-da-paz M, Dorea JG, Galdino AS, et al. Carcinoembryonic antigen (CEA) and hepatic metastasis in colorectal cancer: update on biomarker for clinical and biotechnological approaches[J]. Recent Pat Biotechnol, 2018, 12(4):269-279. doi: 10.2174/1872208312666180731104244 [11] 杨晓虹,李昂,傅传刚,等.结直肠癌根治术后5年内脑转移的危险因素分析[J].第二军医大学学报,2017,38(8):993-996. [12] Cong ZJ, Hu LH, Ji JT, et al. A long-term follow-up study on the prognosis of endoscopic submucosal dissection for colorectal laterally spreading tumors[J]. Gastrointest Endosc, 2016, 83(4):800-807. doi: 10.1016/j.gie.2015.08.043 [13] 郭佳.血清IL-6、CRP、CA19-9和CEA在胃癌患者中的检测意义[J].湖南师范大学学报 (医学版),2016,13(5):63-66. [14] 李楠,毛夕保,丁晨旻,等.18F-FDG SPECT/CT显像联合CA15-3、CA125和CEA诊断乳腺癌术后复发和(或)转移[J].现代肿瘤医学,2015,20(23):3477-3481. doi: 10.3969/j.issn.1672-4992.2015.23.032 [15] 姜巧丽,樊浩然,赵东亮.血浆D-二聚体和纤维蛋白原对结直肠癌患者手术后生存状况的预测效果[J].四川生理科学杂志,2020,42(2):147-150. [16] 李佳乐,刘旭.D-二聚体在肿瘤中的研究进展[J].国际检验医学杂志,2017,38(18):2588-2590. doi: 10.3969/j.issn.1673-4130.2017.18.031 [17] 施磊,李海,杨银学.联合检测直肠癌患者D-二聚体、CEA和CA199的临床意义[J].宁夏医科大学学报,2016,38(9):1028-1030. [18] 李世龙,张宝,周秀艳,等.D-二聚体和纤维蛋白原降解产物联合检测对肝脏肿瘤的临床意义[J].中国药业,2014,23(16):36-37. [19] 王静,袁玉军.术前CEA、D-二聚体、纤维蛋白原与结直肠癌临床病理特点、分期及预后相关性研究[J].国际检验医学杂志,2019,40(6):690-693. doi: 10.3969/j.issn.1673-4130.2019.06.013 [20] 张成大,何君,黄婷,等.结直肠癌患者血清CEA和D-二聚体检测临床意义[J].中华肿瘤防治杂志,2018,25(4):282-286. [21] Guizado TR. Analysis of the structure and dynamics of human serum albumin[J]. J Mol Model, 2014, 20(10):2450. doi: 10.1007/s00894-014-2450-y [22] 曹静,吕文艳.血清白蛋白表达水平在结直肠癌化疗患者预后评估中的应用价值[J].结直肠肛门外科,2017,23(6):749-752. [23] 吴勇,刘弋.结直肠癌中ICAM-1 和VCAM-1 的表达和临床意义[J].安徽医科大学学报,2015,50(8):1124-1127. [24] 岑小宁,黄许森,韦维,等.结直肠癌患者血清miR-542-3p和miR-203水平及临床意义[J].河北医药,2020,42(1):46-49. doi: 10.3969/j.issn.1002-7386.2020.01.010 [25] Chen X, Chen XG, Hu X, et al. MiR-34a and mir-203 inhibit surviving expression to control cell proliferation and survival in human osteosarcoma cells[J]. J Cancer, 2016, 7(9):1057-1065. doi: 10.7150/jca.15061 -




 下载:
下载: