A new system for tumor evaluation and decision-making in elderly patients withcancer
-
摘要: 中国已进入老龄化社会,而恶性肿瘤即是衰老疾病的一种。恶性肿瘤在老年人群中发病率普遍偏高,衰老和肿瘤存在一定的内在联系。老年肿瘤患者具有其独特性,如伴随疾病、多重用药、虚弱状态、认知障碍等,限制了常规抗肿瘤治疗模式在老年这一特殊人群中的应用。故而,老年肿瘤患者的治疗决策很大程度上依赖于完善的动态老年评估,完善的评估可预测老年肿瘤患者是否可从常规抗肿瘤治疗模式中获益。此外,因伦理要求,多数临床研究设置了入组年龄上限,基于此所获之临床证据难以指导高龄肿瘤患者的临床实践,故亟需在该领域有所创新。本文就上述领域的研究现状及发展趋势进行综述,并针对老年肿瘤人群的全面评估和精准临床决策进行讨论。Abstract: China’s population is aging, and cancer is an aging-related disease. The incidence of malignant tumors is generally high in the elderly. There is a fundamental link between aging and cancer. In addition, elderly patients with cancer have unique characteristics, such as comorbidities, polypharmacy, frailty, and cognitive impairment, which limit the application of conventional anti-tumor therapies in this special population. Therefore, treatment decision-making for elderly cancer patients is largely dependent on excellent dynamic geriatric assessment, which can predict whether these patients will benefit from conventional anti-tumor therapies. Furthermore, due to ethical requirements, most clinical studies set an upper age limit for enrollment. Based on this clinical evidence, clinical management of elderly patients with cancer is difficult, and innovations in this field are urgently needed. This article reviews the current research and development trends in the aforementioned area and discusses the comprehensive evaluation and accurate clinical decision-making for elderly patients with cancer.
-
Key words:
- elderly patients /
- cancer /
- evaluate /
- decision making
-
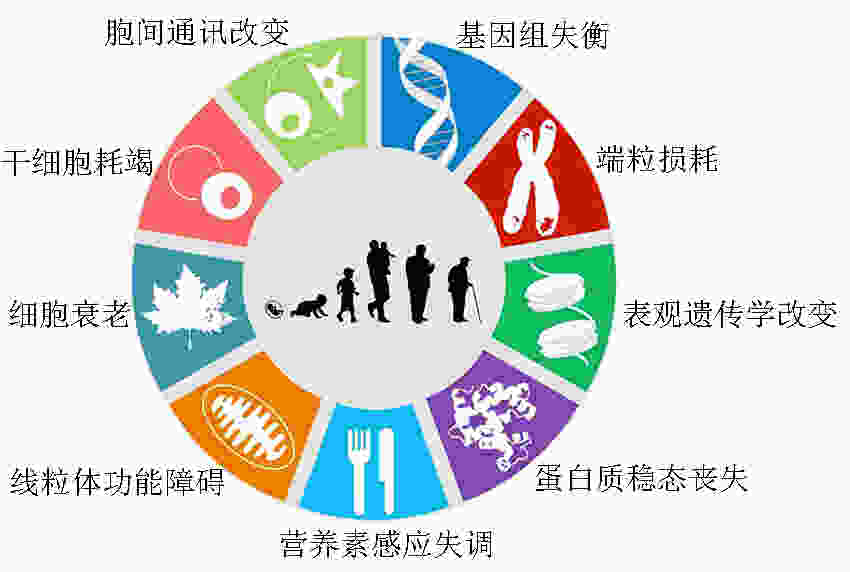
图 1 衰老的9大特征[3]
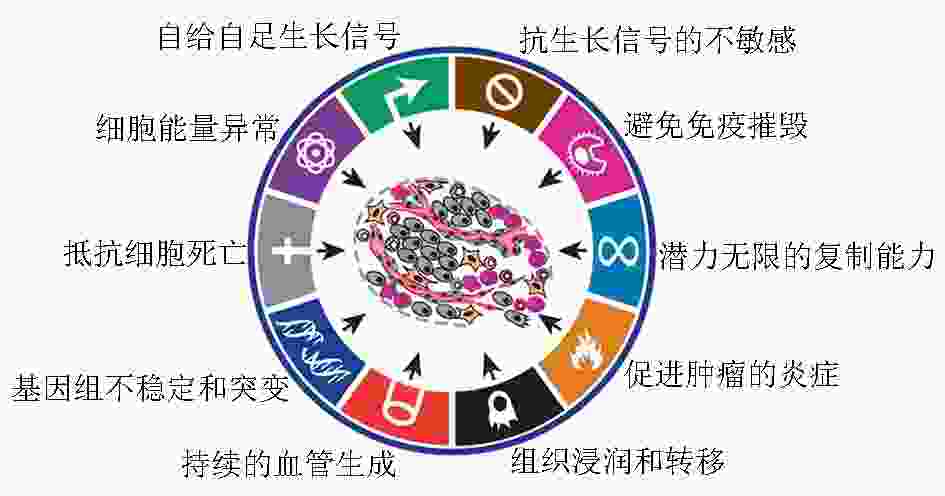
图 2 肿瘤的10大特征[4]
-
[1] Chen WQ, Zheng RS, Baade PD, et al. Cancer statistics in China, 2015[J]. CA Cancer J Clin, 2016, 66(2):115-132. doi: 10.3322/caac.21338 [2] Berger NA, Savvides P, Koroukian SM, et al. Cancer in the elderly[J]. Trans Am Clin Climatol Assoc, 2006, 117:147-155. [3] López-Otín C, Blasco MA, Partridge L, et al. The hallmarks of aging[J]. Cell, 2013, 153(6):1194-1217. doi: 10.1016/j.cell.2013.05.039 [4] Hanahan D, Weinberg RA. Hallmarks of cancer: the next generation[J]. Cell, 2011, 144(5):646-674. doi: 10.1016/j.cell.2011.02.013 [5] Purohit S, Zhi WB, Ferris DG, et al. Senescence-associated secretory phenotype determines survival and therapeutic response in cervical cancer[J]. Cancers (Basel), 2020, 12(10):E2899. doi: 10.3390/cancers12102899 [6] Cho H, Mariotto AB, Mann BS, et al. Assessing non-cancer-related health status of US cancer patients: other-cause survival and comorbidity prevalence[J]. Am J Epidemiol, 2013, 178(3):339-349. doi: 10.1093/aje/kws580 [7] Edwards BK, Noone AM, Mariotto AB, et al. Annual Report to the Nation on the status of cancer, 1975-2010, featuring prevalence of comorbidity and impact on survival among persons with lung, colorectal, breast, or prostate cancer[J]. Cancer, 2014, 120(9):1290-1314. doi: 10.1002/cncr.28509 [8] Gross CP, McAvay GJ, Krumholz HM, et al. The effect of age and chronic illness on life expectancy after a diagnosis of colorectal cancer: implications for screening[J]. Ann Intern Med, 2006, 145(9):646-653. doi: 10.7326/0003-4819-145-9-200611070-00006 [9] Mohile SG, Fan L, Reeve E, et al. Association of cancer with geriatric syndromes in older Medicare beneficiaries[J]. J Clin Oncol, 2011, 29(11):1458-1464. doi: 10.1200/JCO.2010.31.6695 [10] Nightingale G, Hajjar E, Swartz K, et al. Evaluation of a pharmacist-led medication assessment used to identify prevalence of and associations with polypharmacy and potentially inappropriate medication use among ambulatory senior adults with cancer[J]. J Clin Oncol, 2015, 33(13):1453-1459. doi: 10.1200/JCO.2014.58.7550 [11] Whitman A, DeGregory K, Morris A, et al. Pharmacist-led medication assessment and deprescribing intervention for older adults with cancer and polypharmacy: A pilot study[J]. Support Care Cancer, 2018, 26(12):4105-4113. doi: 10.1007/s00520-018-4281-3 [12] Balducci L, Yates J. General guidelines for the management of older patients with cancer[J]. Oncology (Williston Park), 2000, 14(11A):221-227. [13] Boakye D, Rillmann B, Walter V, et al. Impact of comorbidity and frailty on prognosis in colorectal cancer patients: a systematic review and meta-analysis[J]. Cancer Treat Rev, 2018, 64:30-39. doi: 10.1016/j.ctrv.2018.02.003 [14] Magnuson A, Mohile S, Janelsins M. Cognition and cognitive impairment in older adults with cancer[J]. Curr Geriatr Rep, 2016, 5(3):213-219. doi: 10.1007/s13670-016-0182-9 [15] Boulahssass R, Gonfrier S, Champigny N, et al. The desire to better understand older adults with solid tumors to improve management: assessment and guided interventions-the French PACA EST cohort experience[J]. Cancers (Basel), 2019, 11(2):E192. doi: 10.3390/cancers11020192 [16] Extermann M, Boler I, Reich RR, et al. Predicting the risk of chemotherapy toxicity in older patients: the Chemotherapy Risk Assessment Scale for High-Age Patients (CRASH) score[J]. Cancer, 2012, 118(13):3377-3386. doi: 10.1002/cncr.26646 [17] Appelbaum PS. Clinical practice. Assessment of patients' competence to consent to treatment[J]. N Engl J Med, 2007, 357(18):1834-1840. doi: 10.1056/NEJMcp074045 [18] Guerard EJ, Deal AM, Chang Y, et al. Frailty index developed from a cancer-specific geriatric assessment and the association with mortality among older adults with cancer[J]. J Natl Compr Canc Netw, 2017, 15(7):894-902. doi: 10.6004/jnccn.2017.0122 [19] Ferrat E, Paillaud E, Caillet P, et al. Performance of four frailty classifications in older patients with cancer: prospective elderly cancer patients cohort study[J]. J Clin Oncol, 2017, 35(7):766-777. doi: 10.1200/JCO.2016.69.3143 [20] Wildiers H, Heeren P, Puts M, et al. International Society of Geriatric Oncology consensus on geriatric assessment in older patients with cancer[J]. J Clin Oncol, 2014, 32(24):2595-2603. doi: 10.1200/JCO.2013.54.8347 [21] Mohile SG, Dale W, Somerfield MR, et al. Practical assessment and management of vulnerabilities in older patients receiving chemotherapy: ASCO guideline for geriatric oncology summary[J]. J Oncol Pract, 2018, 14(7):442-446. doi: 10.1200/JOP.18.00180 [22] Hamaker ME, Te Molder M, Thielen N, et al. The effect of a geriatric evaluation on treatment decisions and outcome for older cancer patients-A systematic review[J]. J Geriatr Oncol, 2018, 9(5):430-440. doi: 10.1016/j.jgo.2018.03.014 [23] Mohile SG, Epstein RM, Hurria A, et al. Communication with older patients with cancer using geriatric assessment: a cluster-randomized clinical trial from the national cancer institute community oncology research program[J]. JAMA Oncol, 2020, 6(2):196-204. doi: 10.1001/jamaoncol.2019.4728 [24] Puts MTE, Sattar S, Kulik M, et al. A randomized phase II trial of geriatric assessment and management for older cancer patients[J]. Support Care Cancer, 2018, 26(1):109-117. doi: 10.1007/s00520-017-3820-7 [25] Corre R, Greillier L, le Caër H, et al. Use of a comprehensive geriatric assessment for the management of elderly patients with advanced non-small-cell lung cancer: the phase III randomized ESOGIA-GFPC-GECP 08-02 study[J]. J Clin Oncol, 2016, 34(13):1476-1483. doi: 10.1200/JCO.2015.63.5839 [26] Muchnik E, Loh KP, Strawderman M, et al. Immune checkpoint inhibitors in real-world treatment of older adults with non-small cell lung cancer[J]. J Am Geriatr Soc, 2019, 67(5):905-912. doi: 10.1111/jgs.15750 [27] Festen S, Kok M, Hopstaken JS, et al. How to incorporate geriatric assessment in clinical decision-making for older patients with cancer. An implementation study[J]. J Geriatr Oncol, 2019, 10(6):951-959. doi: 10.1016/j.jgo.2019.04.006 [28] Welaya K, Loh KP, Messing S, et al. Geriatric assessment and treatment outcomes in older adults with cancer receiving immune checkpoint inhibitors[J]. J Geriatr Oncol, 2020, 11(3):523-528. doi: 10.1016/j.jgo.2019.05.021 [29] Loh KP, Mohile SG, Epstein RM, et al. Willingness to bear adversity and beliefs about the curability of advanced cancer in older adults[J]. Cancer, 2019, 125(14):2506-2513. doi: 10.1002/cncr.32074 [30] Seymour MT, Thompson LC, Wasan HS, et al. Chemotherapy options in elderly and frail patients with metastatic colorectal cancer (MRC FOCUS2): an open-label, randomised factorial trial[J]. Lancet, 2011, 377(9779):1749-1759. doi: 10.1016/S0140-6736(11)60399-1 [31] Hall PS, Swinson D, Cairns DA, et al. Efficacy of reduced-intensity chemotherapy with oxaliplatin and capecitabine on quality of life and cancer control among older and frail patients with advanced gastroesophageal cancer: the GO2 phase 3 randomized clinical trial[J]. JAMA Oncol, 2021, 7(6):869-877. doi: 10.1001/jamaoncol.2021.0848 [32] Hall PS, Lord SR, Collinson M, et al. A randomised phase II trial and feasibility study of palliative chemotherapy in frail or elderly patients with advanced gastroesophageal cancer (321GO)[J]. Br J Cancer, 2017, 116(4):472-478. doi: 10.1038/bjc.2016.442 [33] Sedrak MS, Freedman RA, Cohen HJ, et al. Older adult participation in cancer clinical trials: a systematic review of barriers and interventions[J]. CA Cancer J Clin, 2021, 71(1):78-92. doi: 10.3322/caac.21638 [34] Liang WH, Guan WJ, Chen RC, et al. Cancer patients in SARS-CoV-2 infection: a nationwide analysis in China[J]. Lancet Oncol, 2020, 21(3):335-337. doi: 10.1016/S1470-2045(20)30096-6 [35] Kuderer NM, Choueiri TK, Shah DP, et al. Clinical impact of COVID-19 on patients with cancer (CCC19): A cohort study[J]. Lancet, 2020, 395(10241):1907-1918. doi: 10.1016/S0140-6736(20)31187-9 [36] Lee LY, Cazier JB, Angelis V, et al. COVID-19 mortality in patients with cancer on chemotherapy or other anticancer treatments: a prospective cohort study[J]. Lancet, 2020, 395(10241):1919-1926. doi: 10.1016/S0140-6736(20)31173-9 [37] UK Coronavirus Cancer Monitoring Project team. The UK Coronavirus Cancer Monitoring Project: protecting patients with cancer in the era of COVID-19[J]. Lancet Oncol, 2020, 21(5):622-624. doi: 10.1016/S1470-2045(20)30230-8 [38] Earl HM, Hiller L, Vallier AL, et al. 6 versus 12 months of adjuvant trastuzumab for HER2-positive early breast cancer (PERSEPHONE): 4-year disease-free survival results of a randomised phase 3 non-inferiority trial[J]. Lancet, 2019, 393(10191):2599-2612. doi: 10.1016/S0140-6736(19)30650-6 [39] Fix OK, Serper M. Telemedicine and telehepatology during the COVID-19 pandemic[J]. Clin Liver Dis (Hoboken), 2020, 15(5):187-190. doi: 10.1002/cld.971 -



 下载:
下载: