Thymosin alpha 1 for patients with hepatocellular carcinoma after radical hepatectomy
-
摘要:
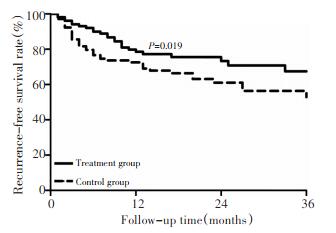
目的 探讨胸腺肽α1(Thymosin alpha 1,Tα1)对肝细胞癌(hepatocellular carcinoma,HCC)患者根治性手术预后的影响。 方法 回顾性分析本院2007年1月至2012年12月558例HCC根治性手术后患者,分为Tα1治疗组146例和空白对照组412例,经倾向性评分匹配后,比较两组术后肝功能恢复情况、无瘤生存率和总生存率。 结果 两组患者共106对匹配成功,中位随访时间为22个月,治疗组较对照组术后TBIL、ALB、ALT、PT等肝功能指标明显改善(P < 0.05)。治疗组和对照组术后1、2、3年无瘤生存率分别为79.7%、70.8%、67.3%和69.9%、61.5%、51.6%(P=0.019);总生存率分别为87.2%、82.0%、68.4%和78.2%、64.2%、49.7%(P=0.011)。 结论 HCC根治术后应用Tα1治疗能有效改善患者术后肝功能,显著提高患者无瘤生存率和总生存率。 Abstract:Objective The effect of thymosin alpha 1 (T α 1) on patients with hepatocellular carcinoma (HCC) after radical hepatectomy was assessed. Methods A total of 558 HCC patients treated by radical hepatectomy were retrospectively collected. Patients in the treatment group (n=146) received postoperative Tα1 therapy, whereas patients in the control group (n=412) did not. Propensity scale matching was conducted to improve the balance between the two groups. Changes in liver function, recurrence-free survival rates, and overall survival rates were compared between the two groups. Results Postoperative liver function (i.e., TBIL, ALB, ALT, and PT) in the treatment group was significantly better than that in the control group (P < 0.05). The one-, two-, and three-year recurrence-free survival rates and overall survival rates in the treatment group were significantly higher than those in the control group (P=0.019 and P=0.011, respectively). Conclusion Postoperative Tα1 therapy can improve postoperative liver function, thus significantly prolonging recurrence-free survival and overall survival. -
表 1 经PSM匹配前后治疗组和对照组的基线资料
Table 1. Baseline characteristics of the treatment and control groups

表 2 治疗组与对照组肝功能变化的比较
Table 2. Comparison of liver function between the treatment group and the control group after operation

-
[1] Forner A, JM Llovet, J Bruix. Hepatocellular carcinoma[J]. The Lan cet, 2012, 379(9822):1245-1255. https://www.mayoclinic.org/diseases-conditions/hepatocellular-carcinoma/cdc-20354552 [2] 柯阳, 钟鉴宏, 游雪梅, 等.抗病毒治疗对乙型肝炎病毒相关性肝细胞癌患者根治性术后的影响[J].中国肿瘤临床, 2013(19):1184-1188. doi: 10.3969/j.issn.1000-8179.20131131Ke Y, Zhong JH, You XM, et al. Antiviral, therapy for hepatitis B vi rus-related hepatocellular carcinoma after radical hepatectomy[J]. Chin J Clin Oncol, 2013(19):1184-1188. doi: 10.3969/j.issn.1000-8179.20131131 [3] 郑江华, 王广义.肝癌术后转移复发相关因素的研究进展[J].实用医学杂志, 2010, 26 (12):2239-2241. doi: 10.3969/j.issn.1006-5725.2010.12.080Zheng JH, Wang GY. Research progression of factors related with postoperative transfer and recurrence in liver cancer[J]. The Journal of Practical Medicine, 2010, 26(12):2239-2241. doi: 10.3969/j.issn.1006-5725.2010.12.080 [4] 黎乐群, 苏智雄, 彭民浩, 等.手术打击对原发性肝癌病人术后免疫功能影响的研究[J].中华肝胆外科杂志, 2004, 10(6):420-421. doi: 10.3760/cma.j.issn.1007-8118.2004.06.022Li LQ, Su LQ, Su ZX, et al. The immune functional affection to Primary liver cancer patients after Surgical strike[J]. Chinese Jour nal of Hepatobiltary Surgery, 2004, 10(6):420-421. doi: 10.3760/cma.j.issn.1007-8118.2004.06.022 [5] Zhong JH, Ma L, Wu LC, et al. Adoptive immunotherapy for post operative hepatocellular carcinoma: a systematic review[J]. Int J Clin Pract, 2012, 66(1):21-27. doi: 10.1111/j.1742-1241.2011.02814.x [6] Matteucci C, Minutolo A, Sinibaldi-Vallebona P, et al. Transcrip tion profile of human lymphocytes following in vitro treatment with thymosin alpha-1[J]. Ann N Y Acad Sci, 2010, 1194:6-19. doi: 10.1111/j.1749-6632.2010.05484.x [7] 程树群, 吴孟超, 陈汉, 等.胸腺肽α1对原发性肝癌术后复发的影响.中华肝胆外科杂志, 2004, 10(9):592-593. doi: 10.3760/cma.j.issn.1007-8118.2004.09.006Cheng SQ, Wu MC, Chen H, et al. Anti-recurrence effects of thy mosin α1 in patients with primary liver cancer after hepatectomy[J]. Chinese Journal of Hepatobiltary Surgery, 2004, 10(9):592-593. doi: 10.3760/cma.j.issn.1007-8118.2004.09.006 [8] 邱福南, 王耀东, 田毅峰, 等.胸腺肽α1治疗对HBsAg阳性肝癌患者根治术后复发和预后的影响[J].中国综合临床, 2010, 26(4): 349-351. doi: 10.3760/cma.j.issn.1008-6315.2010.04.006Qiu FN, Wang YD, Tian YF, et al. Efficacy of anti-biral therapy using thymosin1 in HBsAg positive hepatocellular carcinoma after hepatectomy[J]. Clinical Medicine of China, 2010, 26(4):349-351. doi: 10.3760/cma.j.issn.1008-6315.2010.04.006 [9] Zhong JH, Ke Y, Gong WF, et al. Hepatic Resection Associated With Good Survival for Selected Patients With Intermediate and Advanced-Stage Hepatocellular Carcinoma[J]. Ann Surg, 2013. [Epub ahead of print]. http://cn.bing.com/academic/profile?id=87ee7087c146020c41d886b7ed20e479&encoded=0&v=paper_preview&mkt=zh-cn [10] 马良, 钟鉴宏, 黎乐群, 等.肝动脉化疗栓塞在肝细胞性肝癌切除术后应用的系统评价[J].中国癌症防治杂志, 2011, 3 (1):74-81. doi: 10.3969/j.issn.1674-5671.2011.01.21Ma L, Zhong JH, Li LQ, et al. Postoperative transarterial chemoem bolization on patients with hepatocellular carcinoma:a systematic re view[J]. Chinese Jouranl of Oncology Prevention and treatment, 2011, 3(1):74-81. doi: 10.3969/j.issn.1674-5671.2011.01.21 [11] Zhong JH, Li H, Li LQ, et al. Adjuvant therapy options following curative treatment of hepatocellular carcinoma:a systematic review of randomized trials[J]. Eur J Surg Oncol, 2012, 38(4):286-295. doi: 10.1016/j.ejso.2012.01.006 [12] Zhong JH, Li le Q, Wu LC, et al. Lamivudine with or without adefo vir dipivoxil for postoperative hepatocellular carcinoma[J]. Co chrane Database Syst Rev, 2011, 7(12):CD008713. doi: 10.1002/14651858.CD008713.pub2/abstract [13] Garaci E, Pica F, Serafino A, et al. Thymosin α1 and cancer: action on immune effector and tumor target cells[J]. Ann N Y Acad Sci, 2012, 1269:26-33. doi: 10.1111/j.1749-6632.2012.06697.x [14] 黎乐群, 彭涛.复发性肝细胞癌的细胞克隆来源及其与复发时间的关系[J].中华肝胆外科杂志, 1999, 5(1):11.Li LQ, Peng T. Relationship between Cells cloned source and recur rence time inRHCC[J]. Chinese Journal of Hepatobiltary Surgery, 1999, 5(1):11. -




 下载:
下载: