Diagnosis and prognosis of cervical lymph node metastases of squamous cell carcinoma of unknown primary site
-
摘要:
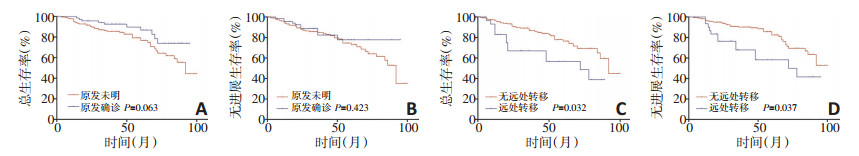
目的 探讨原发病灶不明颈淋巴结转移鳞癌(cervical lymph node metastases of squamous cell carcinoma of unknown primary site,SCCUP)人群发病特点、诊断方法、原发灶检出及预后。 方法 回顾性分析2002年10月至2016年6月天津医科大学肿瘤医院262例SCCUP患者临床病理学特点及预后。运用χ2检验分析原发确诊组与原发未明组的临床表现、原发病灶出现特点及检查方法的灵敏性、特异性,分析影响总体生存期(overall survival,OS)及无进展生存期(progression-free survival,PFS)的因素。 结果 262例SCCUP患者,以男性多见,中位年龄57岁。70例患者检出原发病灶(26.7%),且男性(30.1%)、单枚(31.0%)、Ⅳ区(39.3%)淋巴结转移的原发灶检出率高于女性(17.4%)、多枚(18.7%)、Ⅱ/Ⅲ区(20.8%)。与传统影像学相比,18FDG-PET/CT(18F-fluorodeoxy? glucose positron emission tomography/computed tomography)检出原发灶的灵敏性、特异性高。生存分析显示,远处转移是影响OS、PFS的独立危险因素,N分期对PFS的影响差异有统计学意义(P < 0.05)。 结论 SCCUP患者中,男性、单枚、下颈淋巴结转移的原发灶检出的比例高,PET/CT检查对SCCUP的诊断及原发灶检出有重要意义,N分期较晚及远处转移提示预后不良。 Abstract:Objective To investigate the characteristics, diagnosis, primary detection, and prognosis of cervical lymph node metastases of squamous cell carcinoma of unknown primary site (SCCUP). Methods This study retrospectively analyzed the clinical features and follow-up data of 262 patients with SCCUP. The Chi-square test were used to analyze the clinical performances, characteristics of primary lesions, and sensitivity and specificity of examinations to identify original lesions. Factors related to the overall survival (OS) and progression-free survival (PFS) were also analyzed. Results The 262 patients with SCCUP comprised more men, with a median age of 57 years. At the follow-up, 70 patients were diagnosed with primary lesions (26.7%), and the detection rates of primary lymph nodes in those who were male (30.1%), with a single lesion site (31%), and with level Ⅳ disease (39.3%) were higher than those in patients who were female (17.4%), with multiple lesion sites (18.7%), and with level Ⅱ/Ⅲ disease (20.8%). Compared with traditional imaging examinations, 18F-fluorodeoxyglucose positron emission tomography/computed tomography (PET/CT) had higher sensitivity and specificity in detecting the primary tumor. Survival analysis showed that distant metastasis was an independent risk factor affecting OS and PFS, and the effect of N stage on PFS was statistically significant. Conclusions In SCCUP patients, the proportion of patients who were male, with a single lesion site, and with cervical Ⅳ lymph node metastasis had higher rates of detection of the primary sites. PET/CT examination is important for the diagnosis of SCCUP, as well as the detection of primary lesions. Advanced N stage and distant metastasis indicated poor prognosis. -
Key words:
- cervical lymph node metastasis /
- diagnosis /
- primary lesion /
- prognosis /
- squamous cell carcinoma
-
表 1 262例SCCUP临床病理学特点

表 2 原发未明组与原发确诊组临床病理学特点比较

表 3 PET/CT与传统影像学对原发病灶检出的对比分析

表 4 SCCUP预后单因素分析

表 5 SCCUP预后多因素分析

-
[1] Arosio AD, Pignataro L, Gaini RM, et al. Neck lymph node metastases from unknown primary[J]. Cancer Treat Rev, 2017, 53:1-9. doi: 10.1016/j.ctrv.2016.11.014 [2] Argiris A, Karamouzis MV, Raben D, et al. Head and neck cancer[J]. Lancet, 2008, 371(9625):1695-1709. doi: 10.1016/S0140-6736(08)60728-X [3] Wang Y, He SS, Bao Y, et al. Cervical lymph node carcinoma metastasis from unknown primary site: a retrospective analysis of 154 patients[J]. Cancer Med, 2018, 7(5):1852-1859. doi: 10.1002/cam4.2018.7.issue-5 [4] Kaaks R, Sookthai D, Hemminki K, et al. Risk factors for cancers of unknown primary site: Results from the prospective EPIC cohort[J]. Int J Cancer, 2014, 135(10):2475-2481. doi: 10.1002/ijc.28874 [5] Jereczek-Fossa BA, Jassem J, Orecchia R. Cervical lymph node metastases of squamous cell carcinoma from an unknown primary[J]. Cancer Treat Rev, 2004, 30(2):153-164. doi: 10.1016/j.ctrv.2003.10.001 [6] Barbora U, Marcela N, Vladimir C, et al. Carcinoma of unknown primary in head and neck region[J]. Klin Onkol, 2018, 31(4):277-281. http://d.old.wanfangdata.com.cn/OAPaper/oai_pubmedcentral.nih.gov_3311942 [7] Mondin V, Ferlito A, Devaney KO, et al. A survey of metastatic central nervous system tumors to cervical lymph nodes[J]. Eur Arch Otorhinolaryngol, 2010, 267(11):1657-1666. doi: 10.1007/s00405-010-1357-1 [8] Muller von der Grun J, Tahtali A, Ghanaati S, et al. Diagnostic and treatment modalities for patients with cervical lymph node metastases of unknown primary site- current status and challenges[J]. Radiat Oncol, 2017, 12(1):82. doi: 10.1186/s13014-017-0817-9 [9] Strojan P, Ferlito A, Medina JE, et al. Contemporary management of lymph node metastases from an unknown primary to the neck: I. A review of diagnostic approaches[J]. Head Neck, 2013, 35(1):123-132. doi: 10.1002/hed.v35.1 [10] Schroeder L, Wichmann G, Willner M, et al. Antibodies against human papillomaviruses as diagnostic and prognostic biomarker in patients with neck squamous cell carcinoma from unknown primary tumor[J]. Int J Cancer, 2018, 142(7):1361-1368. doi: 10.1002/ijc.v142.7 [11] Cheol Park G, Roh JL, Cho KJ, et al. (18) F-fdg pet/ct vs. human papillomavirus, p16 and epstein-barr virus detection in cervical metastatic lymph nodes for identifying primary tumors[J]. Int J Cancer, 2017, 140 (6):1405-1412. doi: 10.1002/ijc.30550 [12] Rollo F, Dona' MG, Pellini R, et al. Cytology and direct human papillomavirus testing on fine needle aspirates from cervical lymph node metastases of patients with oropharyngeal squamous cell carcinoma or occult primary[J]. Cytopathology, 2018, 29(5):449-454. doi: 10.1111/cyt.2018.29.issue-5 [13] Luo WJ, Feng YF, Guo R, et al. Patterns of EBV-positive cervical lymph node involvement in head and neck cancer and implications for the management of nasopharyngeal carcinoma T0 classification[J]. Oral Oncol, 2019, 91:7-12. doi: 10.1016/j.oraloncology.2019.01.012 [14] Geltzeiler M, Doerfler S, Turner M, et al. Transoral robotic surgery for management of cervical unknown primary squamous cell carcinoma: Updates on efficacy, surgical technique and margin status[J]. Oral Oncol, 2017, 66:9-13. doi: 10.1016/j.oraloncology.2016.12.033 [15] Di Maio P, Iocca O, De Virgilio A, et al. Role of palatine tonsillectomy in the diagnostic workup of head and neck squamous cell carcinoma of unknown primary origin: A systematic review and meta-analysis[J]. Head Neck, 2019, 41(4):1112-1121. doi: 10.1002/hed.v41.4 [16] Davies- Husband CR. Tongue base mucosectomy for carcinoma of unknown primary using endoscopic electrocautery: rationale for wider implementation of an institutionally restricted technique[J]. J Laryngol Otol, 2018, 132(12):1138-1142. doi: 10.1017/S0022215118002062 [17] Winter SC, Ofo E, Meikle D, et al. Trans-oral robotic assisted tongue base mucosectomy for investigation of cancer of unknown primary in the head and neck region. The UK experience[J]. Clin Otolaryngol, 2017, 42(6):1247-1251. doi: 10.1111/coa.2017.42.issue-6 [18] Bakhshayesh Karam M, Doroudinia A, SafaviNainee A, et al. Role of FDG PET/CT scan in head and neck cancer patients[J]. Arch Iran Med, 2017, 20(7):452-458. http://cn.bing.com/academic/profile?id=da32c08f8ac93f1730633ccf4df0e043&encoded=0&v=paper_preview&mkt=zh-cn [19] Bochtler T, Loffler H, Kramer A. Diagnosis and management of metastatic neoplasms with unknown primary[J]. Semin Diagn Pathol, 2018, 35(3):199-206. doi: 10.1053/j.semdp.2017.11.013 [20] Noij DP, Martens RM, Zwezerijnen B, et al. Diagnostic value of diffusionweighted imaging and (18)F-FDG-PET/CT for the detection of unknown primary head and neck cancer in patients presenting with cervical metastasis[J]. Eur J Radiol, 2018, 107:20-25. doi: 10.1016/j.ejrad.2018.08.009 [21] Kang CJ, Lin CY, Yang LY, et al. Positive clinical impact of an additional PET/CT scan before adjuvant radiotherapy or concurrent chemoradiotherapy in patients with advanced oral cavity squamous cell carcinoma[J]. J Nucl Med, 2015, 56(1):22-30. doi: 10.2967/jnumed.114.145300 [22] Varadhachary GR, Raber MN, Matamoros A, et al. Carcinoma of unknown primary with a colon-cancer profile-changing paradigm and emerging definitions[J]. Lancet Oncol, 2008, 9(6):596-599. doi: 10.1016/S1470-2045(08)70151-7 -




 下载:
下载: