-
摘要:
目的 分析2015年江苏省肿瘤登记地区结直肠癌发病和死亡情况。 方法 依据中国肿瘤登记中心制定的质控方法和评价标准,江苏省疾病预防控制中心对江苏省42个肿瘤登记处上报的2015年全年肿瘤登记资料进行审核和评价,将35个符合质控标准的肿瘤登记处资料汇总成库。按城乡、性别及年龄组分层,计算结直肠癌发病(死亡)率、年龄别发病(死亡)率、累积发病(死亡)率(0~74岁)和截缩发病(死亡)率(35~64岁);采用2000年中国普查标准人口构成和Segi's世界标准人口构成计算中国人口标化率(中标率)和世界人口标化率(世标率)。 结果 2015年江苏省35个肿瘤登记地区覆盖人口38 761 144人(城市15 168 594人,农村23 592 550人),新发结直肠癌病例11 051例,发病率为28.51/10万,中标率为15.43/10万,世标率为15.20/10万,累积发病率(0~74岁)为1.81%,截缩发病率(35~64岁)为23.71/10万;城市地区发病率为33.87/10万,中标率为18.44/10万;农村地区发病率为25.06/10万,中标率为13.54/10万。2015年因结直肠癌死亡5 436例,死亡率为14.02/10万,中标率为6.92/10万,世标率为6.81/10万,累积死亡率(0~74岁)为0.70%和截缩死亡率(35~64岁)为8.08/10万;城市地区死亡率为16.57/10万,中标率为8.27/ 10万;农村地区死亡率为12.39/10万,中标率为6.07/10万。 结论 2015年江苏省结直肠癌发病和死亡水平均呈上升趋势,城市与农村之间存在差异,疾病负担呈逐年加重趋势,应加强结直肠癌的预防和控制工作。 Abstract:Objective To analyze the incidence and mortality of colorectal cancer in Jiangsu province in 2015. Methods Based on the method and criteria of data quality control from the National Central Cancer Registry, data in 2015 from 42 cancer registries in Jiangsu were evaluated by the Jiangsu Provincial Center for Disease Control and Prevention. Data from 35 registries were qualified after assessment and accepted as pooled data. Stratified by urban-rural, gender, and age groups, the crude rates of colorectal cancer incidence and mortality, age-standardized incidence/mortality rates, age-specific incidence/mortality rates, cumulative incidence/mortality rate (0-74 years old), and truncated age-standardized incidence/mortality rate (35-64 years old) were calculated. The Chinese population census in 2000 and Segi's standard world population were used for age-standardized incidence/mortality rates. Results The 35 cancer registries covered a population of 38, 761, 144 (15, 168, 594 in urban areas, 23, 592, 550 in rural areas) in Jiangsu province in 2015. The number of new cases of colorectal cancer were 11, 051, with a crude incidence rate of 28.51/105. The age-standardized incidence rates by the Chinese Standard Population (ASRC) and World Standard Population (ASRW) were 15.43/105 and 15.20/105, respectively. The cumulative incidence rate (0-74 years old) was 1.81%, with a truncated age-standardized incidence rate (35-64 years old) of 23.71/105. The crude and ASRC incidence rates in urban areas were 33.87/105 and 18.44/105, respectively, whereas those in rural areas were 25.06/105 and 13.54/105, respectively. The number of deaths due to colorectal cancer was 5, 436, with a crude mortality rate of 14.02/ 105. The ASRC, ASRW, cumulative (0-74 years old), and truncated (35-64 years old) mortality rates were 6.92/105, 6.81/105, 0.70%, and 8.08/105, respectively. The crude and ASRC mortality rates in urban areas were 16.57/105 and 8.27/105, respectively, whereas those in rural areas were 12.39/105 and 6.07/105, respectively. Conclusions There remains a heavy burden of colorectal cancer in Jiangsu. The incidence and mortality of colorectal cancer show a rising trend in Jiangsu in 2015. The burden and patterns of colorectal cancer show urban-rural differences. Preventative and control strategies should be implemented. -
Key words:
- colorectal cancer /
- incidence /
- mortality /
- Jiangsu
-
表 1 2015年江苏省结直肠癌登记数据主要质量控制指标

表 2 2015年江苏省结直肠癌发病情况

表 3 2015年江苏省结直肠癌死亡情况

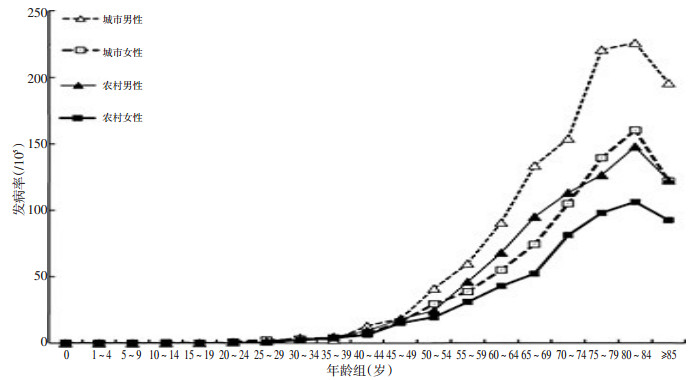
表 4 2015年江苏省结直肠癌年龄别发病率(1/105)

表 5 2015年江苏省结直肠癌年龄别死亡率(1/105)

-
[1] Bray F, Ferlay J, Soerjomataram I, et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries[J]. CA Cancer J Clin, 2018, 68(6):394-424. doi: 10.3322/caac.v68.6 [2] Chen YS, Xu SX, Ding YB, et al. Colorectal cancer screening in high-risk populations: a survey of cognition among medical professionals in jiangsu, china[J]. Asian Pac J Cancer Prev, 2014, 14(11):6487-6491. http://cn.bing.com/academic/profile?id=9808f677995181cdd5d509b0967e0e9c&encoded=0&v=paper_preview&mkt=zh-cn [3] 韩仁强, 武鸣, 俞浩, 等.2010年江苏省肿瘤登记地区恶性肿瘤发病与死亡[J].江苏预防医学, 2015, 26(1):5-10. http://d.old.wanfangdata.com.cn/Periodical/jsyfyx201501002 [4] 韩仁强, 武鸣, 罗鹏飞, 等.2014年江苏省恶性肿瘤发病和死亡分析[J].肿瘤预防与治疗, 2018, 31(1):24-31. doi: 10.3969/j.issn.1674-0904.2018.01.005 [5] 国家癌症中心.中国肿瘤登记工作指导手册[M].北京:人民卫生出版社, 2016:59-75. [6] Forman D, Bray F, Brewster DH, et al. Cancer incidence in five continents, volume X[M]. Lyon; Geneva: International Agency for Research on Cancer; Distributed by WHO Press, World Health Organization, 2014:20-40. [7] James SL, Abate D, Abate KH, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990-2017: a systematic analysis for the Global Burden[J]. Lancet, 2018, 392(10159):1789-1858. doi: 10.1016/S0140-6736(18)32279-7 [8] Roth GA, Abate D, Abate KH, et al. Global, regional, and national agesex-specific mortality for 282 causes of death in 195 countries and territories, 1980-2017: a systematic analysis for the Global Burden of Disease Study 2017[J]. Lancet, 2018, 392(10159):1736-1788. doi: 10.1016/S0140-6736(18)32203-7 [9] Kyu HH, Abate D, Abate KH, et al. Global, regional, and national disability-adjusted life-years (DALYs) for 359 diseases and injuries and healthy life expectancy (HALE) for 195 countries and territories, 1990- 2017: a systematic analysis for the Global Burden of Diseases Study 2017[J]. Lancet, 2018, 392(10159):1859-1922. doi: 10.1016/S0140-6736(18)32335-3 [10] Chen W, Zheng R, Baade PD, et al. Cancer statistics in China, 2015[J]. CA Cancer J Clin, 2016, 66(2):115-132. doi: 10.3322/caac.21338 [11] 武鸣, 韩仁强.江苏省恶性肿瘤报告(2016)[M].南京:南京师范大学出版社, 2017:20-120. [12] 赫捷, 陈万青.中国肿瘤登记年报2016[M].北京:清华大学出版社, 2017: 59-204. [13] 刘晓雪, 宇传华, 周薇, 等.中国近30年间结直肠癌死亡趋势分析[J].中国癌症杂志, 2018, 28(3):177-183. http://d.old.wanfangdata.com.cn/Periodical/zgazzz201803002 [14] Liu S, Zheng R, Zhang M, et al. Incidence and mortality of colorectal cancer in China, 2011[J]. Chin J Cancer Res, 2015, 27(1):22-28. http://d.old.wanfangdata.com.cn/Periodical/zgzl201401003 [15] 武鸣, 周金意.江苏省慢性病及其危险因素监测报告(2013)[M].南京:南京师范大学出版社, 2016:29-98. [16] Brenner H, Kloor M, Pox CP. Colorectal cancer[J]. Lancet, 2014, 383 (9927):1490-1502. doi: 10.1016/S0140-6736(13)61649-9 [17] Gu M, Huang Q, Bao C, et al. Attributable causes of colorectal cancer in China[J]. BMC Cancer, 2018, 18(1):38. doi: 10.1186/s12885-017-3968-z [18] Young GP, St John DJ, Winawer SJ, et al. Choice of fecal occult blood tests for colorectal cancer screening: Recommendations based on performance characteristics in population studies- A WHO (World Health Organization) and OMED (World Organization for Digestive Endoscopy) report[J]. AM J Gastroenterol, 2002, 97(10):2499-2507. http://cn.bing.com/academic/profile?id=6150fd0b91960d66717e033b3051cf5e&encoded=0&v=paper_preview&mkt=zh-cn [19] Moreno CC, Jarrett T, Vey BL, et al. Patient knowledge regarding colorectal cancer risk, opinion of screening, and preferences for a screening test[J]. Curr Probl Diagn Radiol, 2019, 48(1):50-52. doi: 10.1067/j.cpradiol.2017.12.011 [20] Lin JS, Piper MA, Perdue LA, et al. Screening for colorectal cancer: updated evidence report and systematic review for the US preventative Services Task Force[J]. JAMA, 2016, 315(23):2576-2594. doi: 10.1001/jama.2016.3332 [21] Yang DX, Gross CP, Soulos PR, et al. Estimating the magnitude of colorectal cancers prevented during the era of screening 1976 to 2009 [J]. Cancer, 2014, 120(18):2893-2901. doi: 10.1002/cncr.28794 [22] Levin TR, Corley DA, Jensen CD, et al. Effects of organized colorectal cancer screening on cancer incidence and mortality in a large community-based population[J]. Gastroenterology, 2018, 155(5):1383- 1391. doi: 10.1053/j.gastro.2018.07.017 -




 下载:
下载: