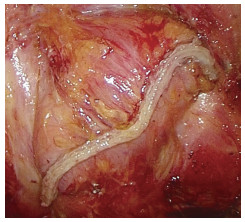
Laparoscopic transabdominal ultra-low anastomosis for rectal cancer: experience of 54 cases
-
摘要:
目的 探讨腹腔镜直肠癌经腹手术超低位吻合保肛的安全性和可行性。 方法 回顾性分析2014年7月至2017年6月西南医科大学附属医院收治的54例行腹腔镜直肠癌根治、超低位吻合患者的临床资料,观察并分析术后疗效。 结果 所有患者顺利完成手术,无中转开腹及手术死亡病例。平均手术时间(165±31)min,术中出血(12±5)mL。本组患者未常规进行预防性造瘘。术后发生吻合口出血2例(3.7%),吻合口漏3例(5.6%),均经保守治疗痊愈。术后患者排尿功能、性功能保持良好,术后一年时绝大部分患者肛门控制排便功能满意,术后随访两年以上均无局部复发,也无死亡病例,但手术一年后有3例患者出现肝脏转移。 结论 腹腔镜直肠癌经腹超低位吻合近期效果良好,远期效果有待进一步观察。 Abstract:Objectives To evaluate the safety and feasibility of ultra-low anastomosis for anal preservation in laparoscopic rectal cancer surgery. Methods The clinical data of 54 patients with low rectal cancer admitted to The Affiliated Hospital of Southwest Medical University from July 2014 to June 2017 were retrospectively analyzed. The short-term effect and complications were analyzed. Results All patients underwent successful operations; conversion to laparotomy or death was not observed in any of the patients. The mean operative time was (165 ±31) minutes, and the intraoperative bleeding volume was (12 ±5) mL. There was no prophylactic ileostomy in all patients. Postoperative anastomotic bleeding and anastomotic leakage occurred in 2 and 3 cases, respectively; these complications were managed with conservative treatment. Postoperative urination and sexual functions of the patients remained good, and most patients were satisfied with their anal function 1 year post-operation. No local recurrences or deaths were noted after follow-up for more than 2 years. However, liver metastases were detected in 3 patients 1 year post-surgery. Conclusions Laparoscopic transabdominal ultra-low anastomosis for rectal cancer has a good short-term effect; however, the long-term effect remains to be evaluated. -
Key words:
- laparoscope /
- rectal cancer /
- ultra-low anastomosis
-
表 1 患者术前cTNM分期情况 例

表 2 患者术后pTNM分期情况 例

-
[1] 郁宝铭.对直肠癌划分高位、中位、低位和超低位临床意义的再认识[J].中华胃肠外科杂志, 2011:14(10):821-822. doi: 10.3760/cma.j.issn.1671-0274.2011.10.31 [2] 徐永强, 邓兵, 罗由平.低位直肠癌的治疗进展[J].四川医学, 2011, 32(5):777-779. doi: 10.3969/j.issn.1004-0501.2011.05.069 [3] 郁宝铭.注意低位直肠癌保肛手术指征的掌握[J].外科理论与实践, 2010, 15(2):89-90. http://d.old.wanfangdata.com.cn/Periodical/wkllysj201002001 [4] Heald RJ. A new solution to some old problems:transanal TME[J]. Tech Coloproctol, 2013, 17(3):257-258. doi: 10.1007/s10151-013-0984-0 [5] Dumont F, Mariani A, Elias D, et al. Surgical strategy for low rectal cancers[J]. JVisc Surg, 2015, 152(1):23-31. [6] 池畔, 陈致奋.腹腔镜不同途径与方法行全直肠系膜切除质量控制评价[J].中国实用外科杂志, 2016, 36(1):28-33. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=zgsywkzz201601011 [7] Chi P, Huang SH, Lin HM, et al. Laparoscopic transabdominal approach partial intersphincteric resection for low rectal cancer:surgical feasibility and intermediate-term outcome[J]. Ann Surg Oncol, 2015, 22(3):944-951. doi: 10.1245/s10434-014-4085-8 [8] 黄颖, 池畔.低位直肠癌行腹腔镜内括约肌切除术技巧与要领[J].中国实用外科杂志, 2017, 37(6):695-698. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=zgsywkzz201706025 [9] 沈荐, 李敏哲, 杜燕夫, 等.腹腔镜直肠癌低位前切除术后吻合口漏的危险因素分析[J].中国微创外科杂志, 2017, 17(10):873-876. doi: 10.3969/j.issn.1009-6604.2017.10.003 [10] Seo SI, Yu CS, Kim GS, et al. The role of diverting stoma after an ultra-low anterior resection foe rectal cancer[J]. Ann Coloproctol, 2013, 29(2):66-71. doi: 10.3393/ac.2013.29.2.66 [11] 秦敬.腹腔镜低位直肠癌保肛术后吻合口漏的危险因素分析及预防对策[J].临床外科杂志, 2017, 25(7):531-533. doi: 10.3969/j.issn.1005-6483.2017.07.017 [12] 彭鸿, 刘琴远, 李庆, 等.低位直肠癌保肛中双吻合术联合保护性回肠造口的疗效观察[J].实用癌症杂志, 2015, 30(9):1357-1359. doi: 10.3969/j.issn.1001-5930.2015.09.028 [13] 马留学, 李景永, 王瑜, 等.三管冲洗引流在预防直肠癌TME术后吻合口漏中的应用[J].中国普通外科杂志, 2011, 20(10):1040-1043. [14] 李晓平, 余绮荷, 李尚仁, 等.术中放置肛管对腹腔镜直肠前切除术吻合口漏的预防作用[J].泰山医学院学报, 2018, 39(6):634-636. doi: 10.3969/j.issn.1004-7115.2018.06.013 -




 下载:
下载: